YOUR PHYSIO
Condition directory
Golfer's elbow
Golfer's elbow is the term used to describe pain arising from the tendons on the inside of your elbow.
The tendons insert onto the medial epicondyle of the humerus (the long bone of the upper arm) as can be seen in the anatomical diagram. This gives the problem its other name which is medial epicondyopathy.
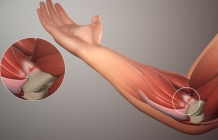
The tendons that insert here are responsible for movements of both the wrist and fingers and are involved in wrist stability during gripping activities.
The main symptoms of golfer's elbow are:
Pain on the inside of the elbow. It is worse on movements of the wrist and gripping activities.It can be worse when first starting to use the arm after a period of rest and then eases off a little.There can be a sensation of stiffness in the tendon first thing on a morning.
It's important to note that you don't need to play golf to have golfer's elbow.
Golfer's elbow can be viewed as any other tendinopathy problem. We will therefore give an overview of what tendons are and why they sometimes develop a problem.
What is a tendon?
A tendon is the end part of a muscle that attaches to bone. It is made up (and looks) different to the rest of the muscle. It is made up mainly of collagen (type 1) which is a very strong, slightly stretchy type of tissue. The tendon isn’t just one piece of collagen, infact it is made up of many tiny fibres. These amazing structures have the capacity to self repair small areas of injury, and can adapt to increasing demand, although they do both of these things very slowly.
Why do we get tendon pain at the elbow?
There are many reasons why we might develop tendon pain- here are the main ones:
The most common reason is a sudden increase in load or activity. Overloading can occur because you do a lot of a new activity, or a one of activity (e.g decorating a room) or you have been exposed to a sudden external force (such as catching yourself if you trip or fall. Because the change is sudden the tendon struggles 'to keep up', leading to pain.
The second most common scenario is constant exposure to overload (i.e sustained heavy activity) for example because of your occupation. Again the tendon is strugling to adapt to the demands you are placing on it. Occupational and lifestyle factors relating to loading are very important in elbow tendinopathy. Infact the ability of the individual to be able to change day to day loading relating to work activity is strongly linked to outcome. People who are able to change or adapt their work activities tend to get better, an inability to change is linked to an increase risk of persistent pain.
Thirdly we may get tendon pain because we don’t use our elbow very often. Tendons can become deconditioned and if they do, normal day to day activities can start to cause changes we normally see with overload.
As you can see the main factor in the development of tendon pain is how the tendon relates to load.
There are however a number of a ‘risk factors’ for tendon pain we need to be aware of.
Some health problems can predispose us to tendon pain for example diabetes, rheumatoid arthritis, depression, and anxiety. It’s important if you have any coexisting health problems that these are well managed.
Lifestyle factors have also been linked to tendon pain. Smoking and being overweight are both associated with a higher likelihood of tendon pain. Why not visit our lifestyle and MSK health page for help managing these risk factors?
What can I do about the problem right now?
1. Deload
If your symptoms have just come on because of a sudden increase in load, they are probably as a result of local inflammation within the tendon. They will usually settle within 6-12 weeks, as long as you are able to ‘deload’ the tendon. This essentially means not repeating the heavy activity again and again, and making sure you modify your day to day activities for a couple of weeks so they don’t cause excessive pain.
If your symptoms are due to constant exposure, then again you may want to ‘deload’. You can do this for example by modifying your work tasks, getting help with heavy lifting, or using more equipment.
A useful technique to employ during this deloading phase is ‘relative rest’.
Relative rest refers to a technique where by you limit your activities based upon your symptoms.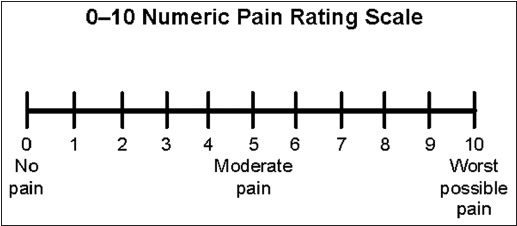
To start with you have to rate your pain on a scale of 0 to 10 where 0 is no pain at all, and 10 the worst pain imaginable. The aim with relative rest is not to let you pain go anymore than 2 points up this scale with your day to day activities (i.e if your rest pain is 2 you should not provoke pain more than 4). This can mean cutting activities short or modifying how you do them for a short period of time. You should apply the principles of relative rest for a few weeks until the pain begins to settle.
If you think you are going to struggle with deloading because of the nature of your job, come and see us. There are other strategies we can employ to achieve deloading which we can teach you, but they do require a detailed face to face assessment.
2. Reload
If you completed the deloading phase or you think you have a tendon underuse problem the next thing to do is to gradually start exposing the tendon to load again.
Why do this? Because these strong amazing structures get their ability to cope with loading by exposure to it. The tendon needs to know in the long term what the normal demand on it is going to be and has to relearn how to cope with this. Once the tendon has ‘settled down’ you can start this gradual education.
The best place to start is with isometric exercises. These are static contractions of the muscle and tendon. These have been shown to reduce short term pain (so are good for self administering pain relief) and help to prepare the tendon for beginning to accept loading through movement.
The video shows you how to do a basic isometric contraction. You should start by only working at about 50% of your maximum push, less if 50% is uncomfortable. Eventually you want to get up to about 70% of your maximum. You should hold the push for about 50 seconds and repeat 2-3 x per day.
What next?
For a good many people simply deloading the tendon and then a simple reloading exercise coupled with a gradual return to normal activity will be enough for their pain to settle.
However some people will reach this stage of being able to perform isometric exercises fine but still have pain. Equally some people will find themselves unable to do this exercise without their symptoms flairing (we call this an irritable tendon). If this is you then speak to your GP about an MSK referral or you can self refer here. The information here represents the first of four phases of tendon rehab that you may need to do. We also have other strategies we can employ if your tendon is really irritable that may allow you to then rehab.
For people with persisting tendon pain it is worth noting that it can take 6 months+ to resolve this, but we can equip you with the tools to take control of the problem and see a good outcome.