YOUR PHYSIO
Condition directory
DeQuervain’s Tenosynovitis
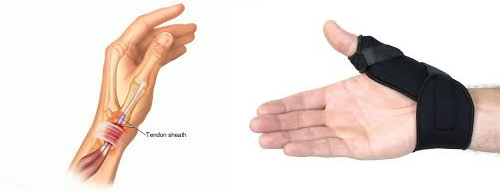
This affects the tendons on the thumb side of the wrist. Pain is felt over the tendons and is often aggravated by repetitive lifting, gripping, or twisting motions of the hand. It can occur after activities involving moving the thumb away from the wrist e.g. hammering or when repeatedly picking a child up.
Treatment
After an initial injury, relative rest in the first instance can help to settle symptoms. Try modifying or reducing provocative activities to allow symptoms to settle. Modifying repetitive work tasks and avoiding heavy lifting is likely to be helpful. Sometimes a splint or a support over the affected area (see picture above) can aid symptoms to settle.
Applying ice, cooling spray or cold gel packs in the early stages can also help symptoms to settle. Use actual ice or a bag of frozen veg wrapped in a cold, damp tea towel or cloth to help the cold conduct really well and help to minimise any risk of ‘cold burn’ to the skin that may occur.
Often non-steroidal anti-inflammatories such as ibuprofen are utilised to help relieve symptoms but these can have a negative effect on tendon healing and the ability of the tendon to adapt to load. It is advised you discuss the use of anti-inflammatories with your GP or pharmacist.
Movement is extremely important to help the tendon heal. A key goal in tendinopathy rehab is improving the capacity of the tendon and muscle to manage load and activity. Modify any activities that bring on your symptoms but gradually introduce exercises and movement and progress these to build up the tolerance of the tendon.
When performing any exercises or activity be guided by how the tendon responds, not just immediately, but also 24 hours later. Tendons are known to have a latent response to loading. This means they can take 24 hours or more to react to it.
Exercises that encourage tendon gliding and gentle loading are shown below; only perform these within a comfortable range and build up only when your symptoms allow. Where possible perform the exercises with both hands at the same time.
Once your pain has settled you can progress your exercises and work on building up your strength.
Should symptoms fail to settle, a corticosteroid injection may be considered to help reduce any inflammation in the area. This would be discussed with you in more detail if required. Your physiotherapist could arrange this if necessary.
If you need additional advice and guidance please complete an MSK self-referral.